Plantar Fasciitis – A Real Pain in the Heel
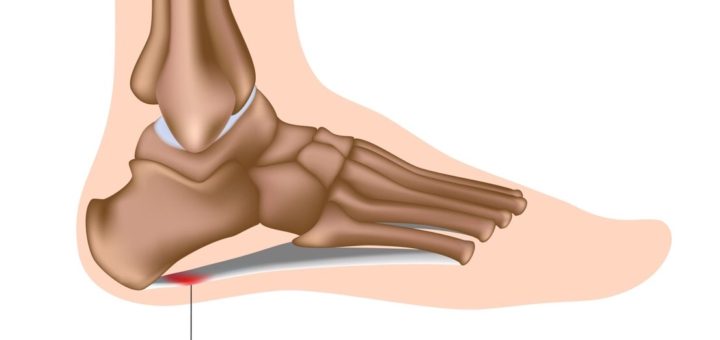
What is Plantar Fasciitis?
Plantar fasciitis is a common cause of heel pain. It’s a stubborn condition, which is difficult to treat. Plantar fasciitis is a degenerative condition of a tough fibrous ligament that helps support the arch of your foot called the plantar fascia.
The pain is felt under the front of the heel, on the inside of your foot, at the insertion of the ligament. The pain varies in severity from mild to severe, tending to be worse after prolonged periods of weight-bearing or exercise. A common feature of plantar fasciitis is that the pain can be at its worst when the ligament is stretched for the first time after a period of resting, such as first stepping out of bed in the morning.
The cause of plantar fasciitis is not exactly known. It is thought to be related to repetitive micro-trauma from overuse, particularly from weight-bearing activities such as walking, running or standing.
Who gets Plantar Fasciitis?
The peak age for plantar fasciitis is between 40 and 60 years of age and it’s slightly more common in women than men. The condition is common in people who stand a lot. It’s also common in runners and sports people who compete on hard surfaces. Physiotherapist, David Wadsworth advises that foot type (ie flat feet or high arches) does not appear to impact someone’s risk for plantar fasciitis. However, in his experience weak calf muscles are often associated with the condition.
Are Heel Spurs on XRays important?
A heel spur is a small bony protuberance from the calcaneus (heel bone) seen on XRay. They are common both in people with plantar fasciitis and without. They are not thought to be relevant to symptoms.
What’s the Best Treatment for Plantar Fasciitis?
Plantar fasciitis is a stubborn condition to treat. It tends to resolve by itself within six to 18 months. It is not dangerous but very inconvenient.
Rest
Physiotherapist, David Wadsworth advises that it is important to reduce the volume of standing, running, jumping and other weight-bearing sport. Be guided by your pain, if what your doing is exacerbating the condition then reduce it.
Orthopaedic surgeon Dr Steven Hatcher warns that recovery can be prolonged.To facilitate complete rest he often recommends crutches for two weeks followed by an immobilisation boot for six weeks before graded return to activities for several months.
Footwear and Orthotics
Using appropriate footwear with arch support and heel cushioning is thought to be beneficial. Also, consider adding a silicone heel gel. Sometimes night splints are used particularly if pain with the first step out of bed is a problem (another eg ‘Strassburg sock‘).
Anti-inflammatory medicines
Anti-inflammatory medicines are thought to be of benefit in managing plantar fasciitis but they are not suitable for everyone. They should be avoided in older age groups, those with high blood pressure, kidney and stomach problems and some asthmatics. Please check with your GP before taking anti-inflammatory medicines.
Topical anti-inflammatory gels that can be rubbed over the site of pain may be an alternative if orals are not suitable but they can cause similar problems so again, check with your GP. Paracetamol is a safe simple pain reliever suitable for most people and it comes in a slow-release preparation for longer lasting effect.
Stretching and Physiotherapy
Your physiotherapist or podiatrist can advise on appropriate stretching, manual therapy and sometimes taping or splinting. Physiotherapist, David Wadsworth advises stretching might include rolling the arch of your foot over a hard object such as a bottle, broomstick or ball and calf stretches. David also recommends calf-strengthening exercises.
Steroid Injection
For more persistent and severe cases, consideration can be given to injection of the heel with a combination of steroid and local anaesthetic. There is reasonable evidence to support that this can give at least short-term relief. It is a painful procedure and there are some risks including infection. Injections can be given in the doctor’s office or under ultrasound guidance and can be repeated as required at intervals (of probably around two to three months). Steroid injections are relatively cheap.
Lithotripsy (ESWT – Extracorporeal shock wave therapy)
Another option for persistent cases is ESWT. This uses powerful sound waves targeted at the plantar fascia insertion. A similar method is used for breaking up kidney stones. It’s unclear exactly how it works but possibly by encouraging regeneration of the ligament. There is quite good evidence to support ESWT use. Repeated treatments are usually required. ESWT is quite expensive.
Platelet-rich plasma (PRP) injections
PRP injection involves injecting blood collected from your veins, which is processed and injected into the plantar fascia. There is moderate level evidence to support PRP injections.
Advanced Sports Clinic – provide both ESWT and PRP
Queensland Lithotripsy Services – provide ESWT
You can expect the cost of a full course of treatment to be around $400 for either of these services as they are not covered by Medicare.
Surgery
Dr Steven Hatcher advises that surgery is an option for persistent and severe cases where symptoms have been present for at least 12 to 18 months and all the more conservative measures have been exhausted. Surgery involves partially releasing the plantar fascia and removing the degenerative tissue.
Plantar fasciitis is not the only cause of heel pain. Please see your GP if you need help with pain in the heel.