Sore Throat
Sore throat is a very common and uncomfortable problem. Here’s a run down on the common causes and treatment.
Pharyngitis (Laryngitis & Bronchitis)
Pharyngitis is a viral infection affecting the pharynx (upper part of the throat). This is the most common type of sore throat and is often accompanied by nasal symptoms, fatigue and fever. It tends to be a mild and self-limiting illness.
Pharyngitis can occur in isolation but is also seen in conjunction with laryngitis and bronchitis. Laryngitis means inflammation or infection of the larynx. Vocal cords are located in the larynx, so laryngitis can cause a hoarse or absent voice for a few days. Bronchitis means infection of the bronchi or larger airways in your lungs. This is experienced as a ‘chesty’ cough, which is sometimes painful, and productive of coloured sputum. The colour of the sputum is not indicative of the need for antibiotics, in fact because this condition is viral it doesn’t respond to them at all.
Treatment of Pharyngitis
The reason sore throat is so unpleasant is that there isn’t a great remedy. Simple painkillers such as Paracetamol or anti-inflammatories can help take the edge off. There are a wide range of products available to help sooth a sore throat such as lozenges, gargles and sprays. Some contain local anaesthetic which numb the throat. Caution must be exercised not to take more than recommended and not to consume hot food or drinks while your throat is numb. Various home-remedies such as hot or cold drinks and gargling saline or Aspirin are also options. Aspirin should be avoided in kids under 16 years of age due to the possible risk of Reye syndrome, which can cause a severe rash. Basically, it boils down to making yourself as comfortable as possible until the illness runs its course, which is usually not more than a few days to a week. Getting extra rest and sleep might be beneficial in not prolonging the illness. These methods can also be used for most other causes of sore throat.
Tonsillitis
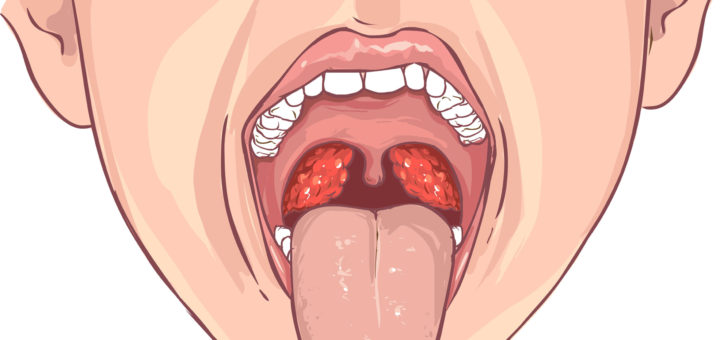
Tonsillitis affects the tonsils, which are collections of lymphatic material at the back of your throat. The adenoids are similar structures but located slightly higher. Tonsillitis can be viral or bacterial. Most cases are viral.
Bacterial tonsillitis
It is not possible to accurately determine if tonsillitis is bacterial or viral by appearances alone. However, your doctor may use certain features to determine how likely the infection is to be bacterial and hence whether you may benefit from antibiotics or not. Bacterial tonsillitis tends to be accompanied by large swollen tonsils coated with pus, fever and tender lymph node swelling in the neck. A cough tends to be absent. If many or all of these features are present your doctor is likely to offer you antibiotics. Throat swabs can be used to more accurately diagnose a bacterial infection but these are not in common use due to practical limitations.
Bacterial tonsillitis can be complicated by such Scarlet fever and rheumatic heart disease. Scarlet fever causes a characteristic rash with pallor around the lips. Rheumatic fever can occur in up to 3 per cent of children with bacterial tonsillitis if not treated with antibiotics and results in joint pains, a rash and damage to the heart valves. Both are treatable with antibiotics.
Glandular Fever (Infectious Mononucleosis)
While most viral tonsillitis is mild and runs a similar course to pharyngitis, a certain type is more well-known for it’s severity and prolonged duration. Glandular fever is caused by the Epstein-Barr virus (EBV). It is spread through saliva such as shared drink bottles, food, kissing and through coughing and sneezing. EBV has a long incubation period, meaning it can take 4-8 weeks from exposure to develop the illness. Also, the virus is shed in salvia for many months after suffering the illness. It tends to cause a sore throat with swollen tonsils, enlarged tender lymph nodes in the neck, armpits and groin. The liver and spleen can become enlarged and less commonly a rash or jaundice (yellow skin) can occur. The major symptoms take 2-3 weeks to settle but fatigue and even depression can last for several weeks longer. Glandular fever is diagnosed with a blood test and treatment is supportive.
Fungal Sore Throat (Candidiasis or Thrush)
Candida causes white growths on the palate and lining of the mouth. It can also cause a metallic taste in the mouth with an unusual sensation of the tongue. It tends to occur in people who use nasal or inhaled steroid sprays (such as for asthma or allergy), after a course of antibiotics, in diabetics, immuno-compromised people and sometimes in those with ill-fitting dentures. Treatment is with anti-fungal lozenges.
Other Infectious Causes of Sore Throat
There are many other important infectious causes of sore throat such as Herpes Simplex (cold sore virus), Diphtheria and Epiglottitis. Epiglottis is caused by a bacteria called Haemophillus influenza and is potentially life threatening due because it can compromise the airway. Thankfully, it is rarely seen since routine immunisation.
Common but less well-known causes of sore throat.
Acid Reflux (Heartburn, Gastro-oesophageal Reflux GOR)
Acid from the stomach sometimes washes up the food pipe (oesophagus) causing a burning sensation and bitter taste in the back of the mouth. It can be exacerbated by too much caffeine, alcohol, spicy food and stress. The reflux can be worse when lying flat so sufferers can experience persistent sore throat that is worse in the morning. Reflux can be treated with lifestyle modification, antacids or prescription acid suppressing tablets. Sometimes an endoscopy is required to exclude Helicobacter pylori infection.
Nasal Congestion and Mouth Breathing
A chronically blocked nose from allergies, nasal polyps or enlarged tonsils or adenoids can result in breathing through the mouth and snoring when asleep. This can cause a persistently sore throat and dry mouth worse in the morning. Treatment can include nasal steroids, antihistamines and surgery. Sleep apnoea must also be considered.
Your GP is an expert in sore throat if you need any further advice.