Guidelines on Managing Hand Injuries for GP’s and Health Professionals.

Five tips from Brisbane hand and upper limb surgeon Dr Pritpal Bansi that could indicate underlying tendon, nerve or artery damage;
- All volar injuries are high risk for tendon, nerve or artery damage and surgical exploration should be strongly considered;
- Always check for paraesthesia, which would indicate nerve damage (before infiltrating with local anaesthetic);
- Always test extension and flexion including separately assessing FDS & FDP function (see below);
- Pain with flexion or extension can indicate partial tendon injury;
- Any puncture wound over a joint, however minor, can potentially seed the joint with bacteria and result in septic arthritis. Serious consideration should be given to surgical exploration of these injuries also.
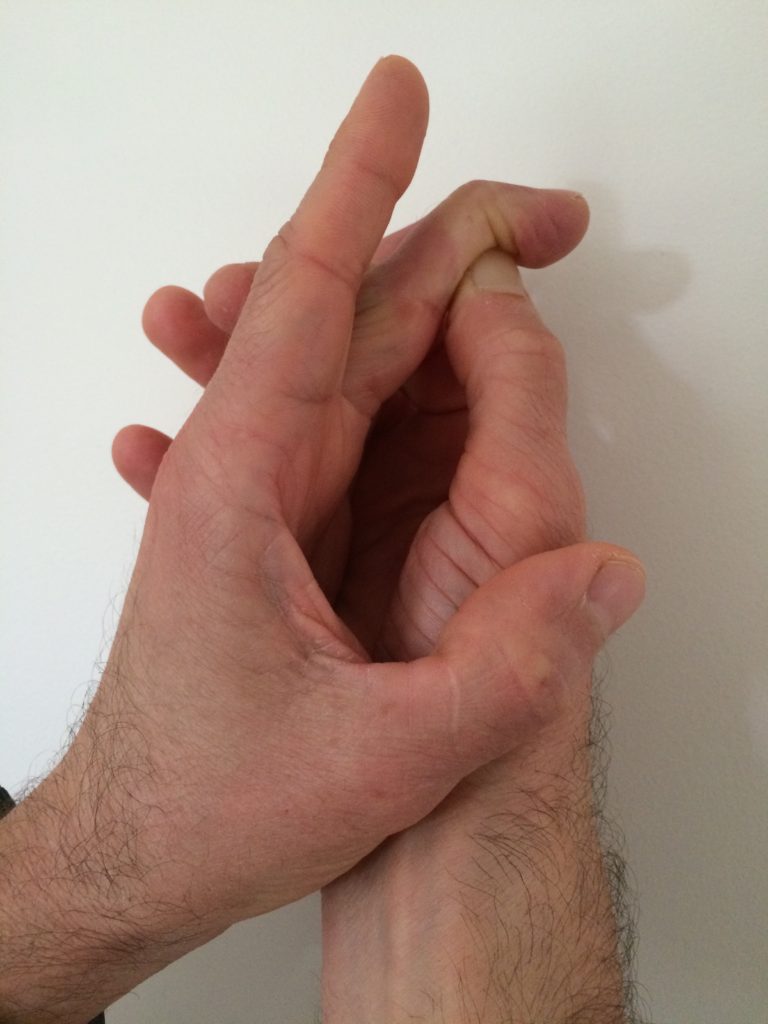
- Testing FDP; mass action, flexes DIPJ
- Testign FDS; flexes PIP, to tests isolate FDP because it can mimic flexion of PIPJ
Volar Finger and Hand Injury Management
Volar finger or hand injuries are more likely to cause unrecognised damage to nerves and flexor tendons than dorsal injuries.
Exploration of a wound under local anaesthetic in the general practice setting may fail to recognise 25-30% of partial or full thickness tendon and nerve injures. Visualisation is often poor due to lack of a tourniquet. Flexor tendons tend to retract remotely from the wound making them difficult to recognise.
Unfortunately, imaging with ultrasound is also notoriously unreliable. Should a patient with a volar injury have full sensation and flexor tendon function (both FDS & FDP) but be unwilling to be referred for surgical exploration a compromise position with explanation and informed consent would be to repair the wound but warn them not to place the tendon under heavy load for a period of six weeks. This would allow any unrecognised partial tendon injury time to heal.
Finally with any injury involving power tools, consideration should be given to X-ray to exclude compound fracture or foreign bodies, which would change management.
Puncture Wound Management
Consideration of surgical exploration should also be given to any puncture wound over a joint, regardless of how minor it appears to be.
Unrecognised joint infection can lead to septic arthritis and destruction of the cartilage. Treatment with antibiotics in the absence of surgical exploration and washout will only suppress infection potentially resulting in delayed diagnosis and permanent loss of the joint surface.
Dorsal Injuries
Dorsal injuries are less-risky as the extensor tendons don’t tend to retract as far into the wound. If under thorough exploration with local anaesthetic no apparent underlying structures are damaged, it is most likely safe to close the wound. Extensor tendons are not under the same load as flexor tendons so delayed rupture is uncommon.
*This is intended as a guide for health professionals only; not for wider public consumption. Please refer to my public post on hand injuries.